Upper Respiratory Infection
Upper respiratory tract infections (URTIs), commonly known as the common cold, represent a significant health concern, particularly in children. These infections are characterized by inflammation of the upper airway mucosa, often caused by viruses or bacteria. While generally mild and self-limiting, URTIs contribute substantially to healthcare resource use due to frequent doctor visits, missed school days, and parental absences from work. In children, URTIs are particularly common, with young children experiencing up to eight episodes per year, while adults average two. The frequency of URTIs decreases as children age. Importantly, the prevalence of URTIs in children poses specific challenges in medical management, especially in the perioperative setting, where it increases the risk of perioperative respiratory adverse events (PRAEs)[1].
Perioperative Respiratory Adverse Events (PRAEs)
PRAEs are a key concern when children with URTIs undergo anesthesia. These complications, which include laryngospasm (involuntary closure of the vocal cords), bronchospasm (narrowing of the airways), and hypoxemia (low blood oxygen levels), among others, can have severe consequences. Studies show that children with active or recent URTI symptoms are at a two to three times higher risk of PRAEs compared to healthy children, with incidence rates ranging from 24% to 30% in affected individuals, compared to 8% to 17% in those without URTIs. These complications can be severe enough to lead to the premature termination of surgery, prolonged oxygen therapy, reintubation, or even admission to the intensive care unit (ICU)[1].
Upper Respiratory Tract Infections (URTIs)
URTIs in children are typically caused by viral agents such as rhinovirus, which is responsible for up to 80% of cases. Other pathogens include respiratory syncytial virus (RSV), parainfluenza, and influenza viruses. Infections like RSV are particularly problematic in vulnerable populations, including immunocompromised children or young infants. RSV, for instance, is linked to increased airway hyperresponsiveness and can contribute to the development of asthma. Such infections necessitate careful perioperative evaluation, as they significantly raise the risk of PRAEs[1].
Diagnosis
The diagnosis of URTIs is usually based on the presence of two or more symptoms, such as rhinorrhea (runny nose), sore throat, sneezing, nasal congestion, malaise, cough, or fever. Other associated symptoms may include muscle pain, headaches, and fatigue. For children with more severe symptoms, such as a green nasal discharge or a moist cough, the risk of experiencing more serious PRAEs, such as bronchospasm or laryngospasm, increases threefold[1].
Surgical Timing
The timing of surgery in relation to URTI symptoms is crucial. Children who undergo surgery within the first two weeks of a URTI are at the highest risk of experiencing PRAEs, due to residual airway inflammation that persists even after symptom resolution. However, after a four-week period, most children return to their baseline risk for respiratory complications. This timeline presents a challenge for healthcare providers when scheduling elective surgeries, as delaying procedures to mitigate risk must be balanced against healthcare resources and other factors.
Management
Medications
In managing children with URTI symptoms perioperatively, both anesthesia techniques and airway management strategies play vital roles in minimizing the risks of PRAEs. Salbutamol is advised for preoperative use in children with current or recent URTIs, as studies indicate significant reductions in PRAEs when administered shortly before anaesthesia induction. Delivery via a spacer in the anesthetic circuit is the optimal approach.[1] Anaesthetic choice becomes critical; intravenous (i.v.) propofol is preferred over inhalational agents due to its effectiveness in reducing PRAEs. Inhalational agents like sevoflurane have some bronchodilator properties but limited effects on airway reflex suppression; thus, they should be utilized with caution.[2] In addition, certain medications, like midazolam, have been associated with higher respiratory risks and should be avoided. Instead, alternatives such as dexmedetomidine, an α2-adrenergic agonist, can be considered to reduce these risks[1].
Airway Techniques
Airway management is another critical aspect of perioperative care in children with URTIs. Endotracheal tubes (ETTs) are associated with a higher risk of PRAEs compared to less invasive devices like laryngeal mask airways (LMAs) or face masks. Consequently, using LMAs instead of ETTs can significantly reduce the incidence of PRAEs, particularly in infants[2][3]. The method of extubation, whether awake or deep, also plays a role in the likelihood of respiratory complications. Though research on the safest extubation approach is mixed, the method should be tailored to each patient's condition and procedure[2].
Scoring Systems/Pre-Operative Assessment
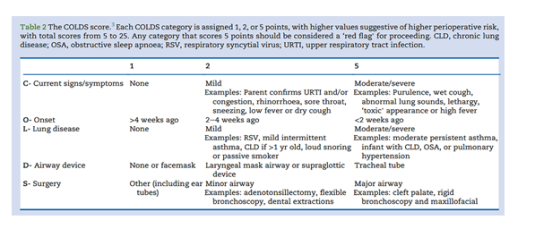
Recent studies have developed tools like the COLDs score to help stratify the risk of PRAEs in children with URTIs. This scoring system takes into account various clinical factors, such as the severity of the URTI symptoms and the child's overall health, to guide decision-making regarding the timing of surgery and the appropriate anesthetic management [1][2]. While useful, such tools are not exhaustive and should be supplemented with clinical judgment, particularly when managing complex cases or urgent surgeries.
History taking and clinical examination are crucial for determining fitness for surgery in children with URTIs. Routine testing for immune markers is generally not recommended.[2] Preoperative assessment in children should emphasize respiratory health and the severity of any respiratory illness. The decision to proceed with surgery should consider the urgency of the procedure versus perioperative risks, with factors like the surgical setting influencing risk tolerance. In complex cases, decision-making should involve a collaborative process between medical professionals and the family, taking into account social factors such as distance from the hospital or the need for care for other children.[1]
Clinical Considerations
Most children with mild URTI can undergo non-major elective surgeries safely, especially in a well-equipped pediatric hospital. Studies have shown that more experienced anesthetists and the absence of severe URTI symptoms reduce the likelihood of perioperative respiratory adverse events. [1]
The global COVID-19 pandemic has introduced additional challenges in managing pediatric patients with URTIs. The virus responsible for COVID-19, SARS-CoV-2, can cause a wide range of respiratory illnesses in children, from mild URTIs to severe complications such as acute respiratory distress syndrome (ARDS) and multiorgan failure. The risk of severe illness increases with age, though young children under four years are most vulnerable to hospitalization, ICU admission, and mortality. Interestingly, many children, especially those vaccinated, may be asymptomatic, serving as silent spreaders of the virus.[1]
The Pediatric AirWay complicationS during COVID-19 (PAWS-COVID-19) study investigated anesthesia-related airway management complications in children with COVID-19. It found that COVID-19-positive children were 2.7 times more likely to experience significant oxygen desaturation during airway management compared to non-infected controls. This risk was even higher for children with symptomatic COVID-19 compared to asymptomatic cases. However, studies have also shown that children generally have a lower risk of perioperative respiratory adverse events and mortality from COVID-19 compared to adults. This is important when considering the balance between delaying elective surgeries and the associated public health burden.[1]
Guidelines now suggest that children with mild COVID-19 can be managed similarly to those with URTI for elective surgery, except where hospital policies demand isolation. One study showed no significant difference in respiratory adverse events between children who delayed elective surgery by 14 or 28 days post-COVID recovery, suggesting that a shorter delay may suffice in many cases. A two-week delay post-symptom resolution can ease pressure on hospital isolation facilities, but shorter protocols may apply if COVID testing is incorporated. Studies in both adults and children have generally recommended a two-week delay after mild COVID-19 and a longer delay after severe illness, particularly for those with significant comorbidities or who are immunocompromised.[1]
Summary
In summary, while children with URTIs or COVID-19 are at an elevated risk of PRAEs during anesthesia, most children undergoing minor elective surgeries can be safely managed with careful perioperative planning. By considering clinical history, symptom severity, and anesthetic techniques, healthcare providers can mitigate the risks of respiratory complications. Risk assessment tools, such as the COLDs score, alongside clinical judgment, can aid in decision-making to ensure the safest outcomes for pediatric patients with URTIs[1][2].
Relevant Article Depot: URI
Upper Respiratory Infections and Airway Adverse Events in Pediatric Procedural Sedation
Anesthesia for the child with an upper respiratory tract infection: still a dilemma? (Review)
Perioperative considerations for the child with an upper respiratory tract infection. (Review)
Upper respiratory tract infections and pediatric anesthesia. (Review)
Should you cancel the operation when a child has an upper respiratory tract infection?
An update on the perioperative management of children with upper respiratory tract infections
Risk assessment for respiratory complications in paediatric anaesthesia: a prospective cohort study
References:
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Preoperative preparation of children with upper respiratory tract infection: a focused narrative review
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 An update on the perioperative management of children with upper respiratory tract infections
- ↑ The effect of endotracheal tubes versus laryngeal mask airways on perioperative respiratory adverse events in infants: a randomised controlled trial