Intraoperative Cardiac Arrest: Difference between revisions
No edit summary |
No edit summary |
||
| Line 1: | Line 1: | ||
'''<u>Incidence of Perioperative Cardiac Arrest (CA):</u>''' | '''<u>Incidence of Perioperative Cardiac Arrest (CA):</u>''' | ||
Increase with | Increase with higher ASA status | ||
Wake Up Safe Registry: 3.3 per 10,000 of arrest were anesthesia related. Aesthesia-related death was 0.36 per 10,000 anesthetics. | Wake Up Safe Registry: 3.3 per 10,000 of arrest were anesthesia related. Aesthesia-related death was 0.36 per 10,000 anesthetics. | ||
| Line 43: | Line 43: | ||
Source: Shaffner DH, Heitmiller ES, Deshpande JK. Pediatric perioperative life support. Anesth Analg. 2013 Oct;117(4):960-979. doi: 10.1213/ANE.0b013e3182a1f3eb. Epub 2013 Sep 10. PMID: 24023023. | Source: Shaffner DH, Heitmiller ES, Deshpande JK. Pediatric perioperative life support. Anesth Analg. 2013 Oct;117(4):960-979. doi: 10.1213/ANE.0b013e3182a1f3eb. Epub 2013 Sep 10. PMID: 24023023. | ||
[[File:PALS Shaffner.jpg|thumb]] | |||
{{Stub Notice}}{{Stub Notice}} | {{Stub Notice}}{{Stub Notice}} | ||
Revision as of 15:48, 18 November 2023
Incidence of Perioperative Cardiac Arrest (CA):
Increase with higher ASA status
Wake Up Safe Registry: 3.3 per 10,000 of arrest were anesthesia related. Aesthesia-related death was 0.36 per 10,000 anesthetics.
Pediatric Perioperative Cardiac Arrest (POCA) Registry: 1.4 +/- 0.45 per 10,000 were anesthesia related. Mortality rate: 26%
Children (<12 year old): 2x more likely to experience CA, infants (<1 year old): 10x, neonates (<1month old): 50x
Causes for Pediatric Perioperative Arrest:
- CIRCULATORY FAILURE:
- Hypovolemia: Hemorrhage, inadequate/inappropriate volume resuscitation/transfusion (patients < 24 months may not respond to hypotension with increase HR)
- Hyperkalemia: Succinylcholine, TRANSFUSION (pRBC >2 weeks, speed of transfusion), reperfusion, myopathy, or renal insufficiency
- Dysrhythmia: LA toxicity, line placement (safer to use Ultrasound guided vs. landmark technique)
- Anaphylaxis
- Venous Air Embolism
- Malignant Hyperthermia: very rare
- RESPIRATORY FAILURE:
- Airway Obstruction: - Laryngospasm: Upper respiratory infection increases risk - Bronchospasm
- Inadequate ventilation and oxygenation: difficult airway, mucus plug, kinked ETT, inadvertent extubation
- Disordered control of breathing: drug overdose, neuromuscular diseases, apnea
- Aspiration
- SUDDEN CARDIAC COLLAPSE
- Bradycardia or cardiovascular collapse: - Traction, pressure, or insufflation involving the abdomen, eye, neck, or heart - Undiagnosed cardiomyopathy
- Overdose - Weight-based dosing of IV anesthetic on induction in a child with hypovolemia or compensated shock may lead to collapse
Important Resuscitation Steps:
- Inform team
- Stop surgical stimulation
- Stop anesthetics (gas & sedation gtt) and vasodilatory meds
- 100% Oxygen
- Open fluids and Trendelenburg position
- Chest-compression
- Call for help
- Consider stopping potassium containing solutions (blood or hyperalimentation)
- Ask for ice to head
- Assign roles
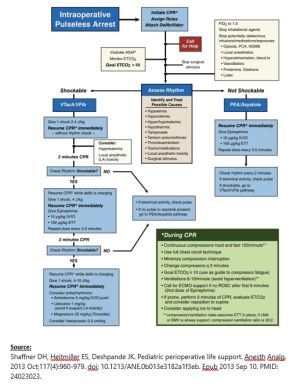
Resuscitation Algorithm:
Source: Shaffner DH, Heitmiller ES, Deshpande JK. Pediatric perioperative life support. Anesth Analg. 2013 Oct;117(4):960-979. doi: 10.1213/ANE.0b013e3182a1f3eb. Epub 2013 Sep 10. PMID: 24023023.
This is a Stub Notice. This page has not been completed. You can work on this page by signing in and going to the Edit tab. Thanks for helping to make PedsAnesthesia.Net Wiki useful.
Go to the Main Page to see the Topic Outline.
Go to the Generalized Suggested Outline for information on case-specific details for each page.
Go to the Test Page for examples on how to use references in the page.
Relevant Article Depot:
This is a Stub Notice. This page has not been completed. You can work on this page by signing in and going to the Edit tab. Thanks for helping to make PedsAnesthesia.Net Wiki useful.
Go to the Main Page to see the Topic Outline.
Go to the Generalized Suggested Outline for information on case-specific details for each page.
Go to the Test Page for examples on how to use references in the page.
Relevant Article Depot: